
Vol. 42, n.º 3, 2009
REVISTA
ESPAÑOLA DE
Vol. 42, n.º 3, 2009 |
CASUÍSTICA
Ricardo Drut
Department of Pathology. «Superiora Sor María
Ludovica» Hospital. School of Medicine, Universidad Nacional de La Plata. La
Plata. Argentina.
patologi@netverk.com.ar
SUMMARY
An unusual location for pyogenic granuloma is reported. The lesions were found during endoscopy in the duodenum of a 13 year old boy with a history of acute myeloid leukaemia and portal hypertension who had undergone a bone marrow transplant. 4 red, raised, polypoid masses measuring 0.7cm were seen in the second and third portions of the duodenum and were resected endoscopically. Histological findings were typical of pyogenic granuloma. To our knowledge, this is the first case report of this condition occurring in the duodenal mucosa of a child.
Key words: Duodenum, pyogenic granuloma.
RESUMEN
En esta presentación se refiere el particular hallazgo de 4 granulomas piogénicos en el duodeno en un paciente pediátrico. Las lesiones fueron halladas en el examen endoscópico de un niño de 13 años con historia de leucemia mieloide aguda, trasplante de médula ósea e hipertensión portal, en forma de pequeñas masas polipoides de 0,7 cm de diámetro en la segunda y tercera porciones del duodeno, procediéndose a su resección en el mismo procedimiento. Los hallazgos histológicos fueron los característicos de este proceso. Este caso parece ser el primero en el que se describen granulomas piógenicos comprometiendo a la mucosa duodenal en un niño.
Palabras clave: Duodeno, granuloma piogénico.
INTRODUCTION
Pyogenic granuloma is a polypoid type of lobular capillary haemangioma whose appearance mimics that of exuberant granulation tissue. It arises most commonly in the skin and oral or nasal mucosa and is only very rarely found in the gastrointestinal tract. Although cases have been reported in both sexes and at all ages, pyogenic granuloma of the gastrointestinal tract in a pediatric patient is extremely unusual. A case of pyogenic granuloma in the duodenum of a child is presented.
CASE REPORT
A 13 year old boy with a history of acute myeloid leukemia (AML) and a bone marrow transplant underwent an endoscopy to monitor oesophageal varices due to portal hypertension secondary to an undefined liver lesion. The endoscopy revealed 4 small, raised, reddish polyps in the second and third portions of the duodenal mucosa which were resected endoscopically.
All four specimens were examined histologically. The polypoid masses consisted of an exophytic proliferation of capillary vessels partially surrounded by oedematous stroma containing inflammatory cells in between local crypts. The surface epithelium was focally eroded and some of the crypts were lined by regenerative epithelial cells (figs. 1 to 4). Immunohistochemistry showed the endothelial cells to be positive for CD31, CD34 (fig. 5) and FVIII, and negative for GLUT-1 and HHV-8. A diagnosis was made of pyogenic granuloma occurring in an unexpected localization.
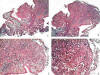
Figs. 1 to 4:
Images depicting the exophytic mass formed by
granulation tissue containing small capillaries with distinctive walls forming
the stroma in between the local crypts. Notice erosion of the surface
epithelium. H&E.
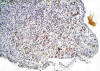
Fig. 5:
CD34 immunostaining highlighting the endothelial
cells of the capillaries.
DISCUSSION
Pyogenic granuloma is a benign lesion of uncertain etiology. Its development has been related mainly to previous local trauma (resulting in an exuberant reactive granulation tissue), hormonal stimuli (it can arise in the skin and oral mucosa of pregnant women), bacterial or viral infections, or arteriovenous anastomosis (1). However, it can also occur in the absence of these conditions.
Pyogenic granuloma is most commonly referred as a polypoid capillary haemangioma, more frequently appearing in the skin and oral or nasal mucosa as a small granulation tissue-like exophytic mass rich in capillaries.
Most cases of pyogenic granuloma of the gastro-intestinal tract have been reported in adults (usually in the 5th and 7th decade of life), and without sex prevalence. The site of the lesions is variable, including esophagus, jejunum, ileum, colon and rectum (2). In the few instances reported in children (3,4,5), the lesions occurred in the colonic and rectal mucosa as well as colostomy mucosa sites. The main clinical finding in all the cases was bleeding, haematemesis, maelena or proctorrhagia, with the resulting anemia.
In the present patient the lesion was found in the duodenal mucosa, a previously unreported site. Another unusual feature of this case was that the lesions were multiple and involved two different sites.
Pyogenic granuloma should be included in the differential diagnosis of polypoid lesions of the bowel such as inflammatory polyp, bacillary angiomatosis and Kaposi sarcoma (6). In the present case the immunohistochemistry was performed merely to highlight the endothelial cells since a definitive diagnosis may be made with just H&E. However, immunohistochemistry for HHV-8 is useful to rule out Kaposi sarcoma, which may imitate pyogenic granuloma (7).
REFERENCES
van Eeden S, Offerhaus GJA, Morsink FH, van Rees BP, Busch ORC, van Noesel CJM. Pyogenic granuloma: an unrecognized cause of gastrointestinal bleeding Virchows Arch, 2004; 444: 590-3.
Yao T, Nagai E, Utsunomiya T, Tsuneyoshi M. An intestinal counterpart of pyogenic granuloma of the skin. A newly proposed entity. Am J Surg Pathol, 1995; 19: 1054-60.
Blanchard SS, Chelimsky G, Czinn SJ, Redline R, Splawski J. Pyogenic granuloma of the colon in children. J Pediatr Gastroenterol Nutrition, 2006; 43: 119-21.
Altamirano E, Drut R. Pyogenic granulomas of the transverse colon. Report of a pediatric case. Patología 2008; 46: 262-4.
Altamirano E, Drut R. Pyogenic granulomas in the ostomy site mucosa. Report of two pediatric cases. Acta GE Latinoam. In press.
González-Vela MC, Val-Bernal JF, Garijo MF, García-Suárez C. Pyogenic granuloma of the sigmoid colon. Ann Diag Pathol, 2005; 9: 106-9.
Urquhart JL, Uzieblo A, Kohler S. Detection of HHV-8 in pyogenic granuloma-like Kaposi sarcoma. Am J Dermatopathol. 2006; 28: 317-21.